Written by Dr Charlotte Keigwin and Dr Anjali Mahto
A recent open-access paper published in The BMJ has generated widespread discussion about the long-term effectiveness of weight loss medication. The authors report that, on average, individuals who discontinue pharmacological treatment for weight management regain the weight they lost within approximately one and a half to two years. This pattern was observed across drug classes, including newer incretin-based therapies such as semaglutide and tirzepatide.
For many people, this finding is unsettling. It can give the impression that weight loss medication offers only temporary benefit, or that weight regained after stopping treatment represents some form of failure. In reality, the paper highlights something far more fundamental: weight loss alters human physiology, and unless those changes are actively managed, reversal is predictable.
Understanding what this study does and does not tell us is essential for anyone considering medical weight loss
The BMJ paper is a systematic review and meta-analysis of 37 randomised and observational studies involving more than 9,000 adults with overweight or obesity. It examines what happens to body weight after weight loss medication is stopped. It does not evaluate comprehensive, long-term weight management services, nor does it assess programmes that address muscle preservation, nutritional adequacy, tissue changes, or maintenance planning. Most included studies treated medication as the primary intervention.

Ref.1
Across studies, weight decreased during active treatment and gradually increased after cessation. When modelled over time, participants returned to baseline weight within an average of 1.7 years. For incretin-based therapies, the estimate was around 1.5 years. These figures reflect population averages rather than individual outcomes, but the underlying biology is well established.
Weight regain in this context is not a behavioural issue. It is a biological response. When weight is lost, the body adapts by reducing resting energy expenditure and increasing hunger signals. These changes evolved to protect against starvation. Appetite-suppressing medication can temporarily counteract some of these signals, but when it is withdrawn, the original regulatory mechanisms reassert themselves.
An additional and often overlooked factor is muscle. If weight loss occurs without attention to muscle preservation, a proportion of the weight lost will be lean tissue rather than fat. Muscle is a major determinant of metabolic rate, glucose handling, and long-term weight stability. Loss of muscle makes weight regain more likely and can contribute to fatigue, weakness, and reduced metabolic resilience.
The BMJ analysis largely reflects models of care in which medication is used without structured support for these physiological changes. This is increasingly relevant as weight loss medication becomes more widely available through services that prioritise access over medical oversight.
For patients, the important question is not whether weight loss medication works, but how it is being used.
Some services focus primarily on prescribing. Assessment may be limited to weight and body mass index. Blood tests, evaluation of metabolic risk, and discussion of muscle or nutrition may be minimal. Follow-up can be light-touch, and there may be little planning for how weight will be maintained if medication is reduced or stopped. In such settings, the pattern described in the BMJ paper is the expected outcome.
Other services take a more comprehensive medical approach. Weight loss medication is used as part of a broader strategy that recognises the complexity of human physiology. Baseline characteristics are assessed more carefully, sometimes including blood pressure, metabolic markers, and nutritional status. Body composition is considered, not just total weight. Muscle preservation and tissue health are addressed alongside appetite and calorie intake.
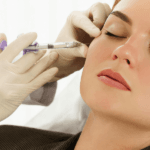
At Self London, weight management is delivered within this second framework. Medication is prescribed by an experienced doctor and integrated into a wider plan designed to reduce predictable risks associated with weight loss. The intention is not simply to achieve weight reduction, but to support the body through that process in a way that is safer and more sustainable.
Muscle preservation is a central part of this approach. Because muscle plays such a critical role in metabolism and long-term weight stability, strategies to support muscle activation are incorporated during weight loss. One such strategy is Pure Impact, a clinically governed neuromuscular stimulation treatment used to activate large muscle groups during periods of reduced caloric intake. Within a weight management programme, its role is to help maintain muscle engagement at a time when muscle loss would otherwise be more likely.
Nutritional adequacy is addressed alongside this. Appetite suppression can make it easier to eat less, but it can also increase the risk of insufficient protein or micronutrient intake. Where appropriate, nutritional input is used to support muscle, energy levels, and overall physiological resilience during treatment.
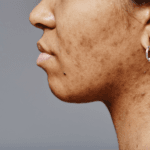
Weight loss also leads to changes in skin and connective tissue, particularly with larger or more rapid reductions. While these changes are not medically harmful, they can influence how people feel about their results and whether weight loss feels sustainable. In selected cases, supportive non-invasive treatments such as Sofwave are used to address tissue laxity by stimulating collagen within the mid-dermis. In this context, Sofwave is not a substitute for weight loss, but a way of supporting tissue quality as the body changes.
An equally important aspect of safe weight management is planning beyond the prescription. Weight loss medication should not be started without considering how long it is likely to be needed, how response will be monitored, and what strategies are available if medication is tapered or stopped. Services with clear clinical governance, defined review points, and structured follow-up are better equipped to manage these transitions.
Seen in this context, the BMJ paper does not argue against weight loss medication. Instead, it highlights the limitations of using medication in isolation. Weight regain after stopping treatment is not a surprise; it is a biological response. Long-term outcomes depend on whether muscle, nutrition, tissue health, and metabolic adaptation are addressed as part of care.
For patients considering treatment, the most useful takeaway from the research is this: weight loss is not a single intervention. It is a physiological process that affects multiple systems in the body. The safety and durability of the outcome depend far more on the medical framework in which medication is used than on the drug itself.
How to choose a safe weight loss clinic
For anyone considering weight loss medication, understanding how to assess the quality and safety of a clinic is crucial. Differences between services are not always obvious at first glance, but they have important implications for both health outcomes and long-term success.
A safe weight loss clinic should be medically led. Weight loss medication affects more than appetite alone; it interacts with blood pressure, glucose regulation, cardiovascular risk, and nutritional status. Prescribing should be overseen by a doctor with appropriate clinical experience, rather than delegated entirely to automated systems or protocol-only models.
Baseline assessment also matters. A clinic should take the time to understand your starting point, not just in terms of weight, but in terms of overall health. This may include blood pressure, metabolic markers, and, where appropriate, blood tests. Without this information, it is difficult to prescribe responsibly or to monitor risk.
Attention to muscle is another important indicator of quality. Rapid weight loss without muscle preservation increases the likelihood of weight regain and can affect strength, energy, and metabolic health. Clinics that consider body composition, rather than focusing solely on the number on the scales, are generally better equipped to support long-term outcomes.
Nutritional support should not be an afterthought. Appetite suppression can make it easier to eat less, but it does not guarantee that what you eat is adequate to support muscle and overall health. A safe service will recognise when nutritional input is needed and address this proactively.
It is also worth asking how a clinic plans for change over time. Weight loss medication is rarely a permanent solution. A responsible service should be able to explain how progress is reviewed, how long treatment might continue, and what options exist if medication is reduced or stopped. Clear follow-up and governance processes are a sign that weight loss is being treated as medical care rather than a short-term product.
Online prescribing and personalised clinical care: understanding the difference
In recent years, weight loss medication has become increasingly available through online platforms. These services typically offer rapid access to treatment, often following completion of a digital questionnaire and, in some cases, a brief remote consultation. For many people, this model is appealing. It is convenient, accessible, and removes the perceived barriers associated with attending a clinic.
However, convenience and clinical depth are not the same thing, and understanding the differences between these models of care is important for patients making decisions about their health.
Online prescribing services are generally designed to streamline access to medication. Assessment is often limited to self-reported information such as weight, height, and medical history, with variable use of objective measurements or blood tests. Follow-up may be automated or infrequent, and care is typically focused on the continuation of medication rather than on broader physiological changes over time. These services are well-suited to scale, but by their nature, they are less able to individualise care or respond to complex or evolving clinical needs.
Personalised, clinic-based weight management takes a different approach. Here, weight loss medication is positioned as one component of medical care rather than the entirety of it. Greater emphasis is placed on baseline assessment, which may include blood pressure, metabolic markers, nutritional status, and consideration of body composition. This allows prescribing decisions to be made in the context of an individual’s overall health rather than solely on eligibility criteria.
Another important distinction lies in how change is managed over time. Weight loss affects multiple systems in the body, including metabolism, muscle, and connective tissue. In a personalised clinical setting, these changes can be anticipated and addressed proactively. Muscle preservation, nutritional adequacy, and tissue support can be integrated into the treatment plan, and adjustments can be made as the body adapts. This is more difficult to achieve in models of care that are designed primarily around medication supply.
Governance and continuity of care also differ. In clinic-based services, there are typically defined review points, clearer lines of accountability, and explicit planning for what happens if medication is reduced or stopped. This matters because weight loss medication is rarely a short, self-contained intervention. Decisions about duration of treatment, maintenance strategies, and long-term health implications benefit from continuity and clinical oversight.
None of this is to suggest that online services are inherently inappropriate. They meet a demand for accessibility and may suit some individuals, particularly those with straightforward needs who are well informed about the limitations of this model. The key issue is alignment between the service model and the complexity of the individual’s situation.
The BMJ paper discussed earlier in this article helps to clarify why these differences matter. Weight regain after stopping medication is not a failure of treatment or motivation; it is a biological response. Services that are designed primarily to initiate medication, without addressing the wider physiological context, are unlikely to alter that trajectory. Services that recognise weight loss as an ongoing medical process, rather than a transactional prescription, are better placed to support safer and more durable outcomes.
For patients, understanding these distinctions can help frame more informed questions. Asking who is prescribing, what assessments are performed, how muscle and nutrition are considered, and what the long-term plan looks like can be more useful than focusing on the medication alone. In weight management, as in much of medicine, how care is delivered is often as important as what is delivered.
References
- Infographic taken from https://www.bmj.com/content/392/bmj-2025-085304