One of the most common questions patients ask is whether they are too young or too old to start injectable treatments. It is usually framed in terms of timing, often influenced by what they see online or among peers, and it assumes that chronological age is the most important factor in deciding when to intervene. While understandable, it is not a particularly useful way to think about treatment. The more relevant question is not when to start, but whether a particular intervention is appropriate in the context of that individual’s anatomy, skin biology and trajectory of change. Many patients who ask this question have already undergone treatments and are trying to understand why the results have not felt quite right.
TL;DR
- There is no “right age” to start injectable treatments. What matters is whether a treatment is appropriate for your anatomy, skin biology and stage of ageing – not your age.
- Facial ageing happens across multiple layers (skin, fat, muscle and bone), so different concerns require different approaches. Skincare alone can’t address deeper structural changes, and injectables are not one-size-fits-all; they each serve distinct roles.
- In younger patients, the focus should usually be on prevention and skin quality (e.g. collagen stimulation, hydration), not adding volume. In older patients, carefully considered structural support may be more appropriate.
- Poor outcomes are rarely about the treatment itself, but about using the wrong intervention, at the wrong time, or in the wrong way. Overuse, especially of filler, can disrupt natural proportions and movement.
- The best results come from accurate diagnosis, restraint and long-term planning. Sometimes, the most appropriate decision is not to treat at all.
Why age is the wrong starting point
This distinction matters because facial ageing does not occur in a single layer, nor does it progress uniformly across individuals or ethnic groups. It is often assumed that ageing is primarily a surface process, something that happens within the skin and can therefore be addressed at that level alone. In reality, the skin is only one component of a much more complex system. Beneath it lie fat, muscle and bone, all of which undergo progressive change over time. These changes alter structural support, volume distribution and the way the face interacts with light, meaning that what appears to be a superficial concern may in fact be driven by deeper anatomical processes.
The layered reality of facial ageing
Facial ageing occurs as a result of several interrelated mechanisms. Photoageing, driven largely by ultraviolet radiation, leads to matrix metalloproteinase-mediated collagen degradation, elastin disorganisation and pigmentary change within the skin. At the same time, the subcutaneous fat compartments beneath the skin begin to thin and separate, a process known as fat atrophy, which disrupts the smooth transitions seen in youth. These compartments are also subject to gravitational redistribution, contributing to descent of tissue and the development of features such as nasolabial folds and jowling. In parallel, the facial skeleton undergoes age-related remodelling and resorption, particularly in areas such as the orbital rim, mandible and pyriform aperture, leading to reduced structural support for the overlying soft tissues. The combined effect is a gradual loss of support, often described metaphorically as the surface becoming too large for the framework beneath it.
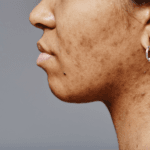
These processes are broadly consistent across all ethnic groups, but the rate at which they occur, and the way they manifest clinically differ. Melanin plays a protective role against ultraviolet radiation, and darker skin types demonstrate significantly higher intrinsic protection compared with lighter skin. The epidermis of Black skin has a UVB protective factor of approximately 13.4 compared with 3.4 in white skin, and for UVA radiation, often associated with photoageing, the figures are approximately 5.7 versus 1.8 respectively. This means that fair skin is more prone to earlier photoageing, often developing fine lines and pigmentary change in the late twenties or thirties, particularly with cumulative sun exposure. Darker skin types, by contrast, may show fewer early surface changes, with ageing becoming more apparent later, often in the fifth or sixth decade.
However, this does not imply that darker skin is resistant to ageing. Rather, the pattern differs. Individuals with more pigmented skin are more likely to experience earlier changes in the mid-face, with descent of the malar fat pad and deepening of nasolabial folds creating a sense of heaviness before fine lines become prominent. This variation reinforces the need to assess not only the presence of ageing but also how it is expressed in each individual, rather than applying a uniform treatment approach.
Different injectables, different biological roles
These underlying processes explain why a purely surface-based approach is often insufficient. While topical skincare and prescription treatments have a role in managing photoageing, they are unable to influence deeper changes in fat or bone. Retinoids can improve fine lines, pigmentation and skin texture, but they do not address structural descent or volume redistribution. This is why concerns such as deep folds, jowls or under-eye hollowing cannot be corrected with skincare alone, regardless of how advanced the formulation may be.
It is within this context that injectable treatments are often introduced, but they are frequently misunderstood as a single category of intervention. In reality, injectables encompass a range of treatments that act at different levels and through different biological mechanisms. Neuromodulators influence muscle activity and are most relevant in contexts where dynamic movement contributes to the development of lines or to early structural change. Repeated contraction of facial muscles creates lines perpendicular to the direction of pull, and over time these dynamic lines can become static. By selectively reducing muscle activity, neuromodulators reduce cumulative mechanical stress on the dermis and can slow this transition. However, muscle function is also integral to expression and facial balance. Overcorrection, or treatment delivered without a clear understanding of underlying muscle interplay, can result in compensatory recruitment of adjacent muscles or a loss of natural movement. The issue is not the treatment itself, but how and when it is used.
Hyaluronic acid fillers, by contrast, are used to restore or redistribute volume where there has been loss or descent of fat. Their role is structural, and when used appropriately they can re-establish support and improve contour. However, volume is not a neutral intervention. It alters proportions and relationships between facial features, and when applied too early or without sufficient regard for underlying anatomy, it can create disproportion rather than correction.
Alongside these sit treatments that are better understood as regenerative or biostimulatory rather than volumising. Polynucleotides act through cellular signalling pathways that support fibroblast activity, tissue repair and modulation of inflammation, creating an environment more conducive to dermal regeneration. Poly-L-lactic acid induces a controlled inflammatory cascade that leads to gradual collagen deposition and dermal thickening over a period of months. Hyaluronic acid–based treatments also exist along a spectrum. Profhilo is best considered a skin booster, improving hydration and dermal environment without materially altering structure, whereas formulations such as Profhilo Structura are designed to provide greater tissue support and sit closer to the biostimulatory end of that spectrum.
Understanding these distinctions shifts the focus away from choosing a product and towards selecting an intervention that matches the biology of the problem. These treatments are not interchangeable, and their effectiveness depends on whether they are used at the correct depth, for the correct indication and at the appropriate stage in the ageing process. It also introduces a temporal dimension that is often overlooked. Some interventions produce immediate changes, while others rely on biological processes such as collagen synthesis that unfold over weeks to months. Without understanding this, patients may misinterpret early results or pursue additional treatment prematurely.
Prevention vs correction: choosing the right timing
In younger individuals, or in those with early signs of ageing, the priority is often to preserve and support the skin rather than to replace volume. Energy-based treatments that stimulate collagen at a dermal level can improve firmness and resilience without altering facial shape, while light-based treatments can address early pigmentation and vascular changes before they become more established. In this setting, technologies such as Sofwave and broadband light therapies such as BBL Forever Young form part of a longer-term strategy to maintain skin quality and delay structural decline. When used correctly, these treatments allow structural and dermal support to be addressed without altering facial proportions, which is often the more appropriate starting point in younger patients.
Injectable treatments can also be used in a way that aligns with this philosophy. Polynucleotides, poly-L-lactic acid–based treatments and hyaluronic acid biostimulators such as Profhilo and Profhilo Structura can support dermal function and improve elasticity without adding volume. Skin boosters can further enhance hydration and resilience. The emphasis is on encouraging the skin to function optimally, rather than compensating for changes that have not yet occurred.
Volume replacement becomes more relevant where there has been demonstrable structural change. Even then, it requires careful consideration. When applied appropriately, it can restore balance and support. When used too early, too aggressively or too broadly, it can create changes that do not align with underlying anatomy. The problem in modern aesthetics is not access to treatment, but the absence of a clear framework for when not to use it.
Why restraint and diagnosis matter more than treatment choice
Humans are highly attuned to facial harmony, often without conscious awareness. We process multiple visual cues when we assess a face, including movement, proportion and structural relationships. When these cues become misaligned, even subtly, it can create a sense that something is not quite right. In aesthetic practice, this may be seen in faces that appear overfilled, lack natural movement, or display a mismatch between skin quality and underlying structure. The issue is not the presence of treatment, but the coherence of the result.
This is why restraint is often a marker of expertise. Treatments performed well tend to be imperceptible. They preserve movement, maintain proportion and respect the underlying anatomy of the face. In many cases, this means doing less or choosing a different type of intervention altogether.
A consultation built on this understanding is not about selecting treatments, but about establishing what is actually required and, just as importantly, what is not. It involves assessing the face as a whole, considering structure, skin quality and the trajectory of change, and deciding whether intervention is appropriate at all. Without that level of clarity, even well-delivered treatments can produce inconsistent results.
At Self London, this is why treatment is not performed on the same day as consultation. Immediate intervention is rarely appropriate in the absence of a clear diagnostic framework. Time allows for reflection, discussion and a more accurate understanding of what will genuinely make a difference, rather than reacting to what feels like an urgent concern in the moment.
It is also worth recognising that outcomes depend not only on the treatment itself, but on the judgement behind it. In The Skincare Bible, published in 2018, I raised the concern that aesthetic treatments were already being overused, including by those working within the field. That observation has only become more relevant. Increased access to treatments has not been matched by the same emphasis on restraint, proportion and long-term thinking.
A critical part of good practice is therefore the ability to recognise when not to treat. This requires an aesthetic eye that remains grounded in what constitutes a healthy, balanced and natural face. It is not a fixed skill. It can be shaped by trends, repetition and prolonged exposure to overtreated results. Without that perspective, it becomes easy to lose sight of what normal ageing actually looks like.
The distinction is not between one treatment and another. It is between a process that begins with treatment selection and one that begins with diagnosis, judgment and considered planning. Ultimately, the question of whether it is “too soon” becomes secondary. What matters is whether the intervention is appropriate, proportionate and aligned with the individual. When that principle guides decision-making, results tend to look less like treatment and more like the person themselves.