Many patients arrive in clinic convinced that their skin was decided at birth. They look at a parent or sibling and assume that their own future is already visible there. Fine lines, pigmentation, a sagging neck and jawline, persistent sensitivity, or “good skin” are framed as inherited traits, largely outside personal control. That belief is understandable, but it is incomplete. Modern dermatology does not support the idea that skin ageing is genetically programmed in a fixed way. Genetics influences how skin behaves, but it does not fully dictate how it will age.
Visible skin ageing results from an ongoing interplay among inherited biology, cumulative exposure (especially ultraviolet light), systemic health, and the skin’s capacity to repair itself. In practice, this is obvious. People with similar genetic backgrounds often age very differently. It usually reflects differences in sun exposure, inflammation, metabolic health, sleep, stress, smoking, and the quality of intervention over time.
Genetics sets a baseline, not a blueprint
Skin traits are not controlled by one decisive gene. There is no single “wrinkle gene” or “good skin gene”. Most visible traits are influenced by many genes, each contributing a small effect. In plain language, your DNA sets tendencies: how readily you burn or tan, how reactive your immune system is in the skin, how robust your barrier function tends to be, how quickly collagen is broken down under stress, and how efficiently your cells repair damage.
Those tendencies matter, but they do not act in isolation. Genes operate through pathways. The pathways that matter most in skin health include collagen synthesis and breakdown, pigment production and distribution, antioxidant defence, inflammation signalling, and DNA repair. The visible outcome depends on what those pathways are exposed to, repeatedly, over decades.
A useful way to think about genetics is that it changes sensitivity. It can make you more vulnerable to certain types of injury or more resilient. It does not determine the amount of injury your skin accumulates, and it does not determine whether you intervene early and intelligently.
Pigmentation genes modify risk, they do not dictate ageing
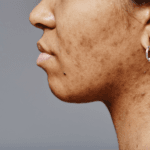
Pigmentation is one of the clearest examples of inherited influence. Variants in genes involved in melanogenesis, the process of making melanin, affect baseline skin colour, how easily you tan, how readily you freckle, and how much natural protection you have against ultraviolet radiation. People who burn easily are not imagining it. Their baseline biology gives them less buffer.
However, within every pigment group there is wide variation in ageing patterns. Two fair-skinned people can have a similar inherited tendency to burn, yet one develops extensive sun damage by midlife while the other does not. The difference is not the gene but it is cumulative exposure. Genetics modifies susceptibility and ultraviolet dose determines outcome.
That is why family history is not a verdict. If you have inherited a tendency to pigment or burn, you simply need to be more disciplined about protection and more precise about treatment when pigment becomes unstable.
Collagen biology is inherited, but structural ageing is modifiable
Structural ageing is driven by what happens in the dermis. Collagen provides tensile strength. Elastin provides recoil. Both are maintained by fibroblasts. In youth, collagen synthesis and breakdown are balanced. With time, synthesis slows and breakdown accelerates. Genetics influences the baseline resilience of this system. Some people inherit thicker dermis, stronger collagen architecture, or a tendency to maintain structure for longer. Others inherit a tendency toward earlier laxity.
But the same pathways that determine collagen balance are strongly influenced by the environment. Ultraviolet radiation increases reactive oxygen species and activates transcription factors that upregulate matrix metalloproteinases, enzymes that degrade collagen. Chronic inflammation does the same. Metabolic dysfunction affects fibroblast behaviour and collagen gene expression. The point is not that genes do not matter. The point is that the forces that act on collagen are, to a large extent, modifiable.
Barrier function and inflammation are genetically influenced but environmentally driven
The skin barrier is not a vague concept but an organised structure of corneocytes and lipids that determines water loss, irritant penetration, and immune reactivity. Some people inherit a barrier that is more prone to dryness or irritation. Some inherit immune tendencies that make them more reactive, which can present as eczema, rosacea, persistent sensitivity, or inflammatory acne.
Yet even in genetically influenced inflammatory disease, the expression is strongly modified by non-genetic inputs. Harsh cleansing, inappropriate actives, frequent barrier disruption, poor sleep, psychological stress, hormonal change, and insulin resistance can all amplify inflammation. In clinic, I often see patients who have labelled their skin as “genetically sensitive” when the dominant issue is a disrupted barrier and chronic low-grade inflammation that has never been stabilised properly.
Epigenetics explains why identical DNA does not mean identical ageing
If genetics were destiny, identical twins would age in lockstep. They do not. Over time, twins often diverge in pigmentation, wrinkling, texture, and laxity. The biological explanation is epigenetics: chemical modifications that control gene expression without changing the DNA sequence.
Ultraviolet radiation, smoking, pollution, persistent inflammation, insulin resistance, and chronic stress all influence epigenetic markers in skin cells. They change which genes are upregulated and which are suppressed. In practical terms, your DNA is the hardware. Epigenetics is the software which is responsive to the environment. This is one reason the idea of an immutable genetic “ageing programme” is outdated. Ageing is the molecular record of lived biology.
Lifestyle is a central biological driver of skin ageing
Lifestyle is not an aesthetic add-on. It is one of the dominant regulators of the pathways that drive dermal breakdown, pigment instability, and impaired repair. A useful way to approach lifestyle in skin is to drop the moral language and focus on mechanisms. When lifestyle matters, it is because it changes signalling in fibroblasts, keratinocytes, melanocytes, immune cells, and the microvasculature.
Insulin resistance and collagen suppression
Fibroblasts are metabolically active cells that depend on insulin signalling via PI3K/Akt pathways to drive collagen gene transcription. In insulin-resistant states, now increasingly common in midlife, this signalling is impaired. Collagen synthesis is downregulated while matrix-degrading enzymes are upregulated. The net effect is that collagen breakdown persistently exceeds collagen production. This is why metabolic ageing accelerates facial ageing independent of sun exposure. Patients with insulin resistance frequently show premature loss of dermal structure even when photodamage is modest.
Insulin resistance also increases oxidative stress and advanced glycation end products. Glycation makes collagen fibres stiffer and more brittle. It contributes to a dull, rigid skin quality that is difficult to correct with topical skincare alone.
Inflammageing and matrix breakdown
Low grade systemic inflammation, sometimes termed inflammageing, is common in midlife. It is driven by visceral adiposity, sedentary behaviour, poor sleep, chronic psychological stress, and metabolic dysfunction. Pro-inflammatory messengers known as cytokines such as IL-6 and TNF-alpha stimulate matrix metalloproteinases and impair normal repair. This is not about obvious redness but rather molecular signalling that accelerates dermal breakdown.
Sleep and circadian repair
Skin repair is circadian. During deep sleep, growth hormone release supports tissue regeneration, and the epidermal barrier is restored. Sleep deprivation reduces this nocturnal repair phase. In controlled studies, poor sleep is associated with slower barrier recovery, greater sensitivity to irritants, and earlier development of fine lines. You cannot out-treat chronic sleep debt with devices.
Stress, cortisol and the barrier
Chronic stress elevates cortisol and sympathetic signalling. Cortisol suppresses fibroblast proliferation, reduces collagen synthesis, and impairs epidermal lipid production. It also increases oxidative stress. Clinically, this often presents as reactive skin, stubborn inflammation, and accelerated ageing.
Muscle, metabolism and facial ageing
Skeletal muscle is a metabolic organ. It influences insulin sensitivity and inflammatory balance. Loss of muscle mass worsens insulin resistance and increases inflammatory signalling. Over time, this indirectly accelerates skin ageing. This is one reason resistance training is relevant to skin health. It supports systemic physiology that underpins collagen maintenance and repair.
What should you do if you have a family history of early ageing, pigmentation, or sensitive skin?
Most patients do not need a genetic test to act intelligently. You need a disciplined, evidence-led approach that targets the pathways your skin is most vulnerable to. In practice, there are a small number of interventions that consistently deliver disproportionate benefit.
First, control ultraviolet dose. Genetics influences how sensitive you are to UV, but UV remains the dominant driver of pigment instability and collagen breakdown. Daily broad-spectrum sunscreen is not a lifestyle slogan. It is the most effective long-term anti-ageing intervention we have. It only works if it is applied in adequate amount and re-applied when exposure is meaningful. If you are prone to pigment, you should also treat visible light and heat exposure seriously, because these can worsen melanocyte instability in some patients.
Second, stabilise the barrier before you chase actives. Reactive skin is often a barrier problem amplified by inflammation, not a mysterious genetic curse. A gentle cleanser, appropriate moisturisation, and avoidance of frequent barrier disruption come first. Only then should you introduce actives such as retinoids or acids, and only at a pace the skin can tolerate. Overuse is one of the common reasons patients believe they have “genetically sensitive” skin.
Third, use a small number of topical actives that have robust evidence. Vitamin A derivatives remain the most biologically meaningful topical intervention for collagen support and epidermal renewal. Antioxidants can reduce oxidative stress. Pigment modulators can stabilise melanocyte behaviour when used correctly. The key is not the number of products. It is consistency and correct use.
Fourth, treat inflammation as an ageing driver. If you have persistent acne, rosacea, eczema, or chronic redness, do not dismiss it as cosmetic. Inflammation upregulates collagen degrading pathways. Medical management of inflammatory skin disease is an anti-ageing intervention in biological terms.
Fifth, do not ignore systemic physiology. If sleep is poor, stress is chronic, alcohol is high, or insulin resistance is developing, the skin will show it. You do not need perfection, but you do need awareness. The goal is to reduce chronic inflammatory load and support repair.
Finally, if you want meaningful change, use clinical tools early rather than waiting for severe damage. Once collagen architecture has degraded and pigment instability is entrenched, correction is slower and more complex.
How Self London turns this biology into a plan, not a protocol
The reason outcomes vary between clinics is simple. Most clinics deliver treatments, but few diagnose biological drivers and then design an integrated plan.
At our medical dermatology clinic on Harley Street, we start by making skin measurable. A VISIA consultation is not a marketing step. It is phenotyping. It allows us to map pigment patterning, vascular activity, texture changes, pore and photodamage signatures, then track change objectively over time. For patients who have been told their skin is “just genetic”, objective imaging often reveals that the dominant issue is cumulative photodamage, chronic inflammation, or barrier disruption. Those are treatable.
When the dominant driver is photodamage and pigment instability, the most effective strategy is to address pigment and vascular signalling, then rebuild dermal structure. This is where BBL and combination platforms, including BBL with HALO when appropriate, are clinically useful. The goal is not a single dramatic treatment. It is a progressive correction: reducing inflammatory vascular signalling, improving pigment stability, and supporting long-term skin quality.
When the dominant driver is dermal collagen loss and early laxity, collagen stimulation has to be approached as biology rather than branding. Technologies such as Sofwave are used to target dermal collagen pathways and induce neocollagenesis over months. The endpoint is not an immediate lift. It is an improved collagen architecture over time, guided by skin phenotype and realistic structural goals.
When repair capacity is low, or where the skin needs support around the eyes, scars, or texture change, we may use biostimulatory approaches. Polynucleotides and other biostimulators are not “injectables” in the cultural sense. They are repair signalling interventions. Used correctly, they can improve tissue quality and resilience and can be combined intelligently with energy-based treatment, rather than offered as a standalone trend.
If systemic metabolic state is contributing, we address that directly. This is where Pure Impact sits within the broader model. It is not a facial treatment. It is a body intervention designed to support muscle, strength, and metabolic health. In practical terms, supporting muscle helps improve insulin sensitivity and inflammatory balance. That systemic effect matters to skin biology, particularly in midlife and in patients who are losing muscle through inactivity, dieting, or weight loss medication. When patients improve strength, sleep and metabolic stability, their skin often becomes more treatable, and results from collagen stimulation and pigment correction improve.
The point is not that everyone needs every intervention. The point is that skin ageing is multi-factorial. The plan has to be as well.
How do you know what you need, and what you should ignore?
A high quality clinic should be able to tell you, in clear terms, what is driving your skin changes and what is unlikely to help. If your main issue is ultraviolet-driven pigment, you need pigment and vascular correction plus protection, not a drawer of products. If your main issue is collagen loss, you need collagen stimulation and time, not repeated superficial facials. If your barrier is disrupted, you need simplification and repair, not escalation. And if inflammation is persistent, it needs medical management, because chronic inflammation accelerates structural ageing.
Genetics influences your baseline. It does not give you a treatment plan. The treatment plan comes from identifying your dominant drivers and then intervening with consistency.
A more precise view of “lifestyle” that patients can actually implement
Patients often ask for lifestyle advice and receive vague recommendations. What matters is reducing the specific biological pressures that accelerate collagen breakdown and pigment instability. In practice, two areas have the highest yield.
The first is glucose stability. You do not need to pursue extreme restriction, but frequent glucose spikes increase oxidative stress and glycation, and over time they reinforce insulin resistance. A simple approach that is realistic for most people is to build meals around protein and fibre first, minimise ultra-processed snacks, and prioritise strength training because it improves insulin sensitivity independent of weight loss. If you already do the basics and your skin still behaves as though it is ageing faster than expected, it is reasonable to consider whether insulin resistance is developing even with a healthy lifestyle, particularly in midlife. That is a medical discussion, not a moral one.
The second is chronic inflammatory load. Persistent low-grade inflammation in skin can come from uncontrolled acne, rosacea, eczema, perioral dermatitis, or repeated barrier disruption. It can also be amplified by smoking, high alcohol intake, poor sleep, or chronic stress. The actionable point is not to eliminate all stress. It is to stop stacking biological stressors. If sleep is consistently poor, the skin’s repair capacity is limited, and device-based collagen stimulation will not perform as well as it should. If inflammatory skin disease is active, controlling it medically is part of an anti-ageing strategy because it reduces the molecular drivers of collagen degradation.
If you want to act on this now
If you are unsure what is driving your skin changes, the highest value first step is objective assessment and a plan. A VISIA-led consultation allows us to identify whether your dominant pattern is pigment and vascular activity, structural change, inflammation, or barrier disruption, and to track response over time. From there, we can advise whether you are best served by a skin health pathway focused on photodamage and pigment, a collagen stimulation pathway (for example Sofwave), a combined approach using light and fractional technology such as BBL and HALO where appropriate, or repair-supporting treatments such as polynucleotides or other biostimulators when the tissue needs additional resilience. If systemic metabolic state is contributing, we will say so, and we can discuss how Pure Impact fits as a body treatment to support strength and muscle as part of a wider longevity strategy.
Genetics is not a life sentence. It is a starting position. What matters is the cumulative biology that follows: ultraviolet dose, inflammatory load, metabolic stability, sleep, and the quality of intervention.