Post-Roaccutane Skincare
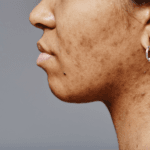
Roaccutane (isotretinoin) is a drug I have both first-hand personal experience of using and vast professional experience of prescribing. It can be used for a variety of skin conditions with acne being the most common (but I will also use it in differing dose regimens for other medical skin problems such as rosacea and hidradenitis suppurative).
I am often asked what a post-Roaccutane skin care regime should look like and I will share with you what I do in clinic with my patients. This is my personal practice and some of you may have treating dermatologists who do things differently, so please bear this in mind. I see acne management with Roaccutane in my clinics as a three-phase process:
PHASE 1:
Switching off the acne with Roaccutane at a target dose of 120-150mg/kg of body weight. This is the generally accepted treatment dose level that most of us adhere to, but there are some studies which treat at higher doses of up to 220mg/kg total dose. This process usually takes about 6 months and ensuring that target doses are met reduces the risk of acne recurrence in the future. One of the problems of taking low-dose treatment for short periods of time is that relapse or recurrence becomes much more likely.
PHASE 2:
After the course is complete (my patients have hit their target doses and clinical response is appropriate), I ask my patients to wait 7-10 days as the drug’s side-effects (in particular, dryness of the skin and lips) start to improve. We then enter the “maintenance” phase. I then prescribe Differin gel (adapalene 0.1%) which is a pharmaceutical-grade retinoid or vitamin A-based cream for acne in the UK. This is to be used at night for a minimum of three months. There are a number of reasons for this; Differin is good for acne maintenance and keeps the skin decongested, helps fade red marks or skin staining as well as aiding improvement of early superficial scars.
I request my patients to use a pea-sized amount at night after cleansing, avoiding the eye area. They start off using the product once or twice weekly (not on consecutive nights) and gradually build up use as tolerated. Twenty minutes later they are asked to moisturise to reduce the irritation the product may cause without diluting down its effects.
My preference is that patients use pharmaceutical grade retinoid for acne maintenance rather than weaker over-the-counter skincare, which is less likely to be as effective. In three months, if they have got on well with Differin, I suggest they remain on it long-term (e.g. 12+ months). If they have not, then I will ask them to stop and switch to a weaker over-the-counter retinol product instead at night (e.g. SkinCeuticals Retinol 0.3% or La Roche-Posay Redermic [R]). These products should not be used whilst pregnant.
So a standard post-Roaccutane routine after finishing treatment looks a bit like this (I do not work for these brands, there is no conflict of interest):
AM
PM
Once Differin is being tolerated well, additional products such as a vitamin C serum can be added before moisturiser in the morning but it is important to remember that the skin is still artificially being dried out to some degree with the Differin Gel. It is important not to over-layer products; keep the skincare simple and let the Differin do its work!
This information is not meant to replace medical advice from your treating doctor. It is an educational post of what I do in my clinic with my Roaccutane patients. I know their full medical history as well as their skin so my plan can be tailored to what will work for them as an individual, as well as taking into account their personal preferences. I cannot give personal or tailored advice to those who are not under my care for legal reasons but if you are currently on the medication and looking for guidance then speak to your treating doctor who knows you.
PHASE 3:
If patients have indented scarring, after 3 months of completion of Roaccutane treatment I will discuss scar treatments if it bothers them. I utilise a variety of methods including laser for this and this process will also be ongoing over a period of months. However, beginning to end, both the acne and scars can be treated if they cause concern.
I hope this was helpful and feel free to share it with anyone you think may find it useful!